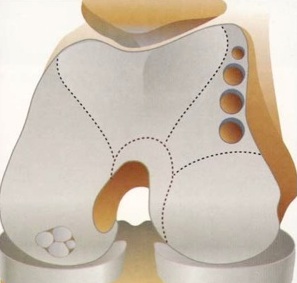
There are many surgical procedures for problems with knee cartilage. Articular cartilage is a white, smooth tissue that covers the bone ends at the area where bones come together to form joints. If cartilage is not healthy, the joints become stiff and painful. Healthy cartilage is necessary for bones to glide across each other without friction.
Articular cartilage is damage from normal wear and tear, injury, trauma, and certain medical conditions. Phoenix orthopedic specialists have perfected many surgical techniques to stimulate the growth of new knee cartilage or to restore cartilage function. These surgical measures can improve mobility, relieve pain, and allow the patient to experience enhanced quality of life.
Chondroplasty
Chondroplasty is a procedure done by arthroscopic technique to smooth the roughened articulate cartilage. This procedure decreases joint friction while preventing thinning of the surface cartilage.
Autologous Chondrocyte Implantation (ACI)
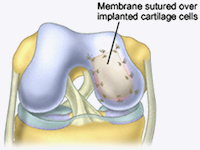
Autologous chondrocyte implantation (ACI) is a two-step procedure. With the first step, healthy cartilage tissue is taken from an area of the patient’s bone that does not have weight-bearing effects, which is done by arthroscopic technique. The tissue contains chondrocytes and is sent to a laboratory where the cells are cultured to increase in number over a period of three to five weeks.
The second step of ACI is done by open surgery (arthrotomy), and the newly grown cells are implanted into the defective area. This procedure is most effective for young patients who have single defects.
Abrasion/Microfracture
Abrasion arthroplasty (also called microfracture) is used for small areas of exposed bone or when there is a complete loss of cartilage. The areas of exposed bone are stimulated to allow bleeding, which leads to the growth of scar cartilage over the area. This cartilage growth permits for a smoother knee joint and improves function. This procedure is done using an arthroscope and is best for younger patients.
The objectives of microfracture are to stimulate new articular cartilage growth and to create better blood supply to the damaged knee area. A surgical tool makes multiple holes in the joint surface beneath the cartilage, creating a healing response. New bone supply reaches the joint surface and brings new cells that form healthy cartilage.
Drilling
Drilling is much like microfracture in that it stimulates the production of healthy cartilage. The orthopedic surgeon will drill multiple holes through the injured area in the subchondral bone. To create a healing response, the subchondral bone is penetrated, and the procedure is easily done by arthroscopic technique. Drilling is less precise than abrasion.
Osteochondral Autograft Transplantation
Osteochondral autograft transplantation involves surgically transferring cartilage from one part of the joint to another region. A healthy cartilage tissue graft is used, and is taken from an area of the bone that is non-weight-bearing. This graft is used as a cylindrical plug of cartilage, which is matched to the surface area of the damaged or defective area. Replacement with the autograft creates a smooth cartilage surface for the knee joint.
Osteochondral autograft is only used for small cartilage defects. Healthy graft tissue can only be removed from a limited joint area. Also, this procedure is often done with an arthroscope.
Tibial and Femoral Osteotomy
Many patients with knee osteoarthritis have damage on either the medial (inside) or lateral (outside) of the knee, or both. This damage causes the knee joint alignment to shift, resulting in knock-knee or bow-leg. Once the alignment is affected, pressure on the knee joint will cause an acceleration of wearing on these areas, and then, more weight is transferred to that knee region. An osteotomy is a realignment procedure done to unload the arthritic side of the knee so the majority of the weight is shifted to the underutilized cartilage. Tibial and femoral osteotomy is performed by adding a bone graft putty to create new bone into the wedged knee region.
Unicompartmental Knee Replacement
When there is severe osteoarthritis of the knee, and conservative measures are not effective, the orthopedic specialist can perform a unicompartmental knee replacement. This invo
lves artificial resurfacing of the cartilage surface, which relieves knee symptoms when the arthritis is limited to only one knee compartment.
Artificial Joint Resurfacing
Artificial joint resurfacing (also called total knee replacement) is a procedure where worn cartilage and bone is replaced with metal and/or plastic pieces. These prosthetic devices are positioned to form an artificial joint surface to alleviate the symptoms of knee arthritis.
Carticel®
Carticel (autologous cultured chondrocytes) is an autologous cellular product. It is indicated for the repair of symptomatic femoral condyle cartilage defects, which occur from repetitive or acute trauma. Carticel is also used for patients who do not respond to other arthroscopic procedures and treatments, and is not indicated for the treatment of cartilage damage related to general osteoarthritis. This product is only used in conjunction with debridement and uses a periosteal flap.
Stem Cells and Tissue Engineering
The latest technology in cartilage treatment involves stem cells and tissue engineering. Growth factors are sued to stimulate new tissue growth and induce cartilage formation. The mesenchymal stem cells are obtained from living human tissue (bone marrow), and are placed at the damaged joint surface to stimulate hyaline cartilage production. Tissue engineering procedures are performed only as part of clinical trials at research centers at this time.