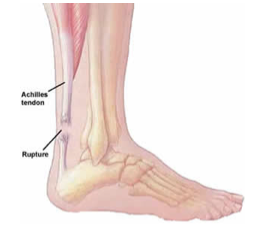
Achilles Tendon Tears
The Achilles tendon represents the common tendon attachment of 3 muscles from the leg: the medial gastrocnemius, the lateral gastrocnemius, and the soleus muscle. The Achilles tendon attaches to the heel bone (or calcaneus) of the foo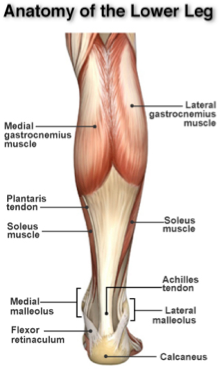 t.
t.
Tears of the Achilles tendon are usually the result of a sudden injury. Often this occurs with running or jumping activities.
Usually there is no history of previous pain in this area but occasionally patients may report a history of chronic pain in the back of the calf or heel prior to the tear.
Signs & Symptoms:
Typically patients who sustain an Achilles tendon rupture report the sudden onset of pain in the posterior calf and often report hearing or feeling a pop. The pain usually subsides gradually with time, but swelling and bruising typically ensue in the days following the injury (see picture below).
Patients also report pain and weakness with attempted walking or pressing the foot down (as if “stepping on a gas pedal”).
The diagnosis of an Achilles tendon tear is typically made by a combination of the patient’s history and the findings on physical examination. X-rays are frequently obtained to rule out other injuries. An ultrasound examination performed in the office will confirm the diagnosis. Occasionally an MRI scan may be used to confirm the diagnosis and determine whether the tear is a partial tear or a complete rupture.
Treatment:
The treatment of Achilles tendon ruptures depends upon the age, health, and activity level of the patient as well as the extent of the tendon injury (ie partial tear versus complete rupture).
For older, less active patients, and those with severe medical problems which preclude safe surgery, non-surgical treat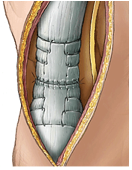 ment is recommended. In addition for patients with partial tears representing less than 50% of the tendon thickness, non-surgical treatment is typically recommended initially. Non-surgical treatment consists of icing, anti-inflammatory medications, casting, activity modifications, physical therapy, and a gradual return to activities as tolerated.
ment is recommended. In addition for patients with partial tears representing less than 50% of the tendon thickness, non-surgical treatment is typically recommended initially. Non-surgical treatment consists of icing, anti-inflammatory medications, casting, activity modifications, physical therapy, and a gradual return to activities as tolerated.
For most active, healthy patients with complete tendon ruptures or partial tendon ruptures which represent more than 50% of the tendon thickness, surgical treatment is recommended. Surgical treatment is ideally performed within 2 weeks from the date of the initial injury before the tendon and muscle begin to scar and shorten and make reattachment it to its native position more difficult. Surgery consists of repairing the ruptured tendon edges back to each other with stitches.