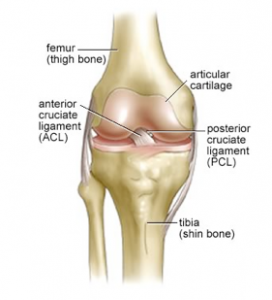
ACL Injury
The anterior cruciate ligament (ACL) is one of the 4 main ligaments in the knee. The ACL combines the thigh bone (femur) to the shin bone (tibia) and target to balance the knee. Although the ACL is not essential for easy actions such as walking, a functioning ACL is required to contribute in activities that engage cutting, twisting, or pivoting.
Injuries to the ACL may occur next sudden acute, twisting episodes. ACL injuries are sometimes related with concomitant injuries to the meniscus (see Meniscus Tears).
Signs & Symptoms:
Typically patients report hearing or feeling a “pop” at the time of injury. Usually patients notice significant swelling over the next 24-48 hours. Although the pain and swelling may decrease, patients with ACL tears often report that their knee feels unstable or “gives out” with certain activities.
Diagnosis:
The diagn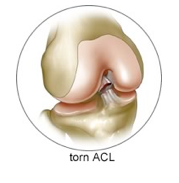 osis of an ACL tear is typically made by a combination of the patient’s history, the findings on physical examination, and an MRI scan.
osis of an ACL tear is typically made by a combination of the patient’s history, the findings on physical examination, and an MRI scan.
Treatment:
Due to the lack of blood supply to the ACL, injuries to the ACL do not heal on their own. In addition, tears of the ACL cannot be repaired by stitching the edges of the tear together. Tears of the ACL must be treated by a surgical reconstruction; in other words, a tissue from somewhere else (either a tissue from your body (called an autograft) or from a cadaver donor (called an allograft)) must be taken and placed in the location of the ACL to create a new ACL.
For more information about autograft and allograft tissue, please go to the ACL graft selection page. Dr. Farber performs this procedure using some of the latest cutting-edge techniques.
See an Overview of ACL Injuries by Phoenix orthopedic surgeon Dr. Adam Farber:
Basics of Accelerated Rehab after an ACL Reconstruction
Following an anterior cruciate ligament (ACL) reconstruction procedure, rehabilitation is imperative. Over the last couple of decades, rehabilitation has improved for patients with ACL injuries. Accelerated rehab after ACL reconstruction was developed as an approach to improve postoperative clinical results. The goal of this rehab is for patients to have full range of motion, excellent stability, and normal function.
Why use Accelerated Rehab?
Thirty years ago, a surgical knee was placed in a cast to avoid excessive stress on the graft. Weight bearing was not allowed for 6-8 weeks after ACL reconstruction, and most patients were not allowed to participate in sporting activities for a full year. This rehab plan brought many postoperative complications, such as knee pain, permanent knee stiffness, and low likelihood of return to high level sports. Because of these complications, doctors and physical therapists devised the accelerated ACL rehab program.
In 1985, researchers analyzed postoperative patients to see why some improved and others did not. They found that patients who moved the knee had fewer long-term knee mobility issues, as well as fewer subjective complaints. They also learned that an early loss of knee extension led to long-term loss of extension, which accompanied pain and stiffness. In addition, they found that patients who failed to regain early knee and leg control had trouble regaining muscle strength later on. They concluded that emphasis should be placed on several factors for rehab: restoration of full hyperextension equal to the opposite knee, allow for early wound healing, and regaining of muscle leg control.
What are the Phases of Accelerated ACL Rehab?
There are five phases involved in accelerated ACL rehabilitation. These include:
Phase 1 – Preoperative: Rehabilitation starts before surgery, immediately following the ACL injury. The goals of Phase 1 include control of swelling before surgery and restoration of normal strength and full range of motion. Patients are educated on the basic principles of accelerated rehab including early weight bearing, strengthening, and full terminal knee extension. This phase last from 1-8 weeks, depending on the initial injury. A cold compression cuff filled with icy water is applied to the knee at this phase. For strengthening, the patients are educated on kinetic chain exercises.
Phase 2 – Immediate Postoperative (0-6 Days): During this phase, goals include decreasing swelling, improving knee flexion, and obtaining full knee extension. Goals include restoring normal walk and performing an independent straight leg raise. To decrease swelling and pain, the cold compression cuff is applied right after surgery. It remains on the knee at all times, except during motion exercises. Continuous passive motion is began immediately using a machine set to 0-30 degrees. This machine stays on the leg at all times. The day after surgery, exercises are performed to improve hyperextension and flexion. The patient remains lying down during the first week, except for going to the bathroom. Crutches are used for normal walking at this time.
Phase 3 – One Week Postoperative (7-14 Days): After a week, the patient visits the physical therapist and surgeon. The rehab program is advanced to concentrate on quadriceps leg control, range of motion, walking, and control of swelling. The cold compression cuff is still used, and the patient is encouraged to progress to full weight bearing without crutches. Leg strengthening exercises increase to facilitate return of lower extremity strength.
Phase 4 – Two Weeks Postoperative (2-4 Weeks): After a couple of weeks, goals include full extension and flexion of the knee, as well as moderate speed strengthening and return to agility and sports drills. Exercises increase and continue to improve range of motion and strength. Patients use a Stairmaster and stationary bike, as well as engage in water activities.
Phase 5 – One Month On: After 4 weeks, the focus is on return to sports and advanced strengthening. This involves full range of motion, regain of 70% of strength, and complete sports function. Patients are encouraged to progress to low repetition/high weights. Activities involve bicycling, swimming, and using the Stairmaster.
Resources
Biggs A, Jenkins WL, Urch SE, & Shelbourne KD (2009). Rehabilitation for Patients Following ACL Reconstruction: A Knee Symmetry Model. N Am J Sports Phys Ther, 4(1), 2-12.
Manske RC, Prohaska D, & Lucas B (2012). Recent advances following anterior cruciate ligament reconstruction: rehabilitation perspectives. Curr Rev Musculoskel Med, 5(1), 59-71.