Chondroplasty is a procedure performed on the damaged cartilage of the knee by the top orthopedic surgeons in Phoenix and Scottsdale. This procedure lessens friction in the joint. Knee chondroplasty can be performed via arthroscopic method to decrease complications, risks, and recovery time.
Who is a candidate for this procedure?
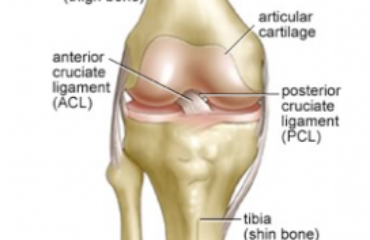
The end of the bones that form the knee joint are covered with articular cartilage, which when smooth, provides  a low friction surface for the knee joint structures. The articular cartilage becomes rough and damaged from arthritis, trauma, and injuries. Damaged knee cartilage causes joint pain and giving way of the knee. These problems are treated using knee arthroscopic chondroplasty.
a low friction surface for the knee joint structures. The articular cartilage becomes rough and damaged from arthritis, trauma, and injuries. Damaged knee cartilage causes joint pain and giving way of the knee. These problems are treated using knee arthroscopic chondroplasty.
How do I prepare for the chondroplasty?
Before surgery, discuss all your medications with the doctor. The doctor will advise you of which medications should be held and which ones to take the day of the procedure. You must not eat or drink after midnight before the surgery, and arrange to have someone drive you home.
How is the procedure performed?
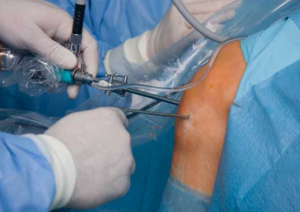
Small incisions are made at the front of the knee by the Phoenix sports medicine physician. A small arthroscope is inserted, which contains a camera and light. This allows the doctor to view inside the joint, and is helpful for diagnosing knee problems. Fluid is pumped into the joint to expand the area. Through the incisions, small instruments are used to remove the loose structures and damaged cartilage tissues. The surfaces is smoothed, and fluid is then drained.
Are there different types of arthroscopy?
The knee arthroscopic procedures include:
- Radiofrequency ablation chondroplasty – Welding over cracks and/or fissures in the articular cartilage).
- Meniscal repair – Resection, trimming, and repair of meniscal tears.
- Abrasion chondroplasty – Shaving of rough damaged cartilage.
- Removal of tissue – Includes loose cartilage and bone fragments.
What can I expect after surgery?
After the procedure, a nurse monitors you in a recovery area for around 45 minutes. You must use crutches and adhere to a strict rehabilitation plan. Exercises are prescribed to help strengthen muscles and improve mobility.
What is involved in the recovery process?
- Bandaging – The doctor makes 3-5 small incisions around the knee, which are closed with sutures an
 d covered with a small bandage. If the bandage becomes saturated with blood and fluid, the dressing can be changed. An ace bandage is used for compression of the knee and must be worn for 2 weeks. Ice packs are recommended several times each day for the first week.
d covered with a small bandage. If the bandage becomes saturated with blood and fluid, the dressing can be changed. An ace bandage is used for compression of the knee and must be worn for 2 weeks. Ice packs are recommended several times each day for the first week. - Sutures – You can remove the dressing after 3 days, but the sutures must be left alone for 14 days. A nurse will remove them at your follow-up appointment.
- Activity – You can bear weight on the leg right after the surgery. Use crutches or a cane if you experience discomfort. You must exercise the quadriceps muscle (front of thigh) to prevent weakening.
- Medication – You are given pain medicine to help with the discomfort associated with surgery. If you do not achieve pain relief, then you should notify the doctor.
- Bathing – After 3 days, you can remove the dressing and take a shower. However, you cannot swim or bathe for 7 days.
What is the success rate of chondroplasty?
In a recent retrospective review involving NBA players, 71% of the players were able to play for several seasons following chondroplasty. In another clinical study, 73% of patients reported improvement after the surgery, and 92% said they would have the procedure again.
Resources
Mithoefer K, Williams RJ 3rd, Warren RF. Chondral resurfacing of articular cartilage defects in the knee with the microfracture technique. Surgical technique. J Bone Joint Surg Am. 2006 Sep;88 Suppl 1 Pt 2:294-304.
Namdari S, Baldwin K, Anakwenze O, et al. Results and performance after microfracture in National Basketball Association athletes. Am J Sports Med 2009 37(5):943-948.