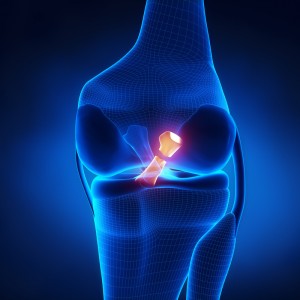
The posterior cruciate ligament (PCL) is a tough band of tissue connecting your thigh bone (femur) to the shin bone (tibia). The PCL is one of four main knee ligaments. A tear in the PCL is a common sports injury.
How common are PCL tears?
PCL tears comprise less than 20% of all knee ligament injuries. Injuries that result in a PCL tear often damage some of the other knee ligaments and cartilage. In certain cases, the posterior cruciate ligament can break loose a piece of
bone underneath where it attaches. In a recent study of the epidemiology of PCL tears, the mean age at the time of injury was found to be 27.5 years. Athletic injuries and traffic accidents accounted for 40% of PCL tears, motorcycle accidents causes 28% of tears, and soccer-related injuries made up 25% of tears.
What causes a posterior cruciate ligament tear?
The most common injury mechanism observed in a recent study was dashboard-related injuries, which accounted for 35% of PCL tears. Another method of injury was fall onto a flexed knee, which accounted for 24% of PCL tears. PCL injuries in sports are often related to a blow to the knee while it is in a bent position.
What sports are associated with PCL tears?
PCL injuries can occur in any sport, but they are most often seen in:
- Football
- Soccer
- Skiing
- Baseball
What symptoms are associated with a PCL tear?
When the injury occurs, most people do not feel or hear a popping sensation or sound, which is common with a tear to the anterior cruciate ligament (ACL). When the PCL is injured, the individual thinks he or she only has a minor knee sprain. However, symptoms later develop, including:
- Wobbly, unstable knee

- Knee pain
- Swelling of the knee
- Trouble walking or bearing weight on the knee
- After some time, a PCL tear may lead to knee arthritis.
How is a PCL tear diagnosed?
The doctor will ask you questions about your injury and conduct a physical examination. The doctor will have you bend your knee, press against a barrier, and check ligament tightness with an arthrometer. In addition, the doctor will ask you to walk around the room. X-rays are used to check for pieces of bone that may have broken loose. The magnetic resonance imaging (MRI) scan is used to confirm the diagnoses of a PCL tear.
The injury is graded based on a simple scale. Grading includes:
- Grade I – The PCL has a small, partial tear.
- Grade II – The PCL is partially torn and loose.
- Grade III – The PCL is complete torn and the knee is unstable.
- Grade IV – The PCL is damaged along with another knee ligament.
How is a PCL tear treated?
Initial treatment involves the PRICE protocol, which includes protecting the knee from further damage, resting the knee, icing the knee for 20-minute intervals, compressing the knee with an elastic bandage, and elevating the knee to decrease swelling. Pain relievers such as ibuprofen are used. While grade I and II injuries do not require surgery, grade III and IV injuries usually do.
The Arizona orthopedic surgeon will reconstruct the PCL arthroscopically, which takes considerable skill. Sometimes, a donor graft is used to replace the torn structure. Dr. Adam Farber at Phoenix Shoulder and Knee has considerable skill and expertise in reconstructing torn PCL’s, while doing so in the most minimally invasive manner possible.
What can I expect during rehabilitation?
After surgery, the length of time for rehabilitation can range from 26 to 52 weeks. Recovery and rehabilitation may include:
- Use of crutches for 2-4 weeks, and then gradually walking on the knee.
- Seeing a physical therapist to help with range of motion, strengthening, and flexibility.
- Wearing a knee brace.
For the top sports medicine treatment in Arizona, call Phoenix Shoulder and Knee today!
Resources
Schulz MS, Russe K, Weiler A, et al. (2003). Epidemiology of posterior cruciate ligament injuries. Arch Orthop Trauma Surg, 123(4), 186-191.