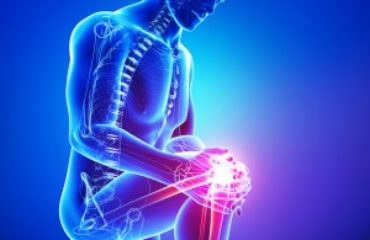
The most common type of knee bursitis is prepatellar bursitis, which involves inflammation of the bursa located at the front aspect of the knee. With kneecap bursitis, localized inflammation and tissue swelling can produce a small lump under the skin.
What causes kneecap bursitis?
Kneecap bursitis is often called housemaid’s knee because it can be caused by:
- Repeated and/or prolonged kneeling – The bursitis develops from frequent microtraumas, which eventually cause inflammation.
- Previous injury – Trauma to the knee can damage the prepatellar bursa, causing it to fill with fluid. When this occurs, the lining
 becomes inflamed.
becomes inflamed. - Medical conditions – Rheumatoid arthritis and gouty arthritis are common causes of kneecap bursitis.
What are the symptoms of kneecap bursitis?
With prepatellar bursitis, the thin, fluid-filled bursa sac becomes inflamed. The bursa serves as a lubricant and cushion between the bone and surrounding tissue. When the bursa fills with fluid, it causes swelling, tenderness, and pain. When bursitis is caused by knee trauma, the symptoms appear suddenly, and within 24 hours. When bursitis is caused from microtrauma (kneeling and repeated motion), the symptoms come on gradually, over 2-4 days or even weeks.
- Localized swelling – Inflamed bursa swells up with fluid, which can be felt through the skin. The knee joint may double in size, feeling squishy to the touch.
- Tenderness and pain – The affected knee can be achy or tender with pressure and movement.
- Decreased range of motion – A swollen bursa can make it hard to flex or extend the knee.
- Warmth and redness – Because of inflammation, the skin over the knee may feel warmer than other body areas, and the color may be pink-red.
How common is prepatellar bursitis?
The annual incidence of prepatellar bursitis is 10 per 100,000 persons. This condition mainly affects men (80%) compared to women (20%), and it is more common among persons 40 to 60 years of age.
What complications are associated with prepatellar bursitis?
Approximately 20% of persons with knee bursitis develop septic bursitis, which means the bursa is infected. Septic bursitis is more common during the summer. People with certain health conditions are more likely to develop septic bursitis, including individuals with diabetes, HIV/AIDS, cancer, alcoholism, lupus, and chronic lung disease.
How is prepatellar bursitis diagnosed?
During the office visit, the Phoenix orthopedic doctor will ask you questions about your symptoms, inquire about your activities, and take a medical history. In addition, the doctor conducts a physical examination takes x-rays of the affected knee. The doctor may also take a fluid sample from the bursa, which is collected using an aspiration technique (arthrocentesis).
How is kneecap bursitis treated?
Kneecap bursitis can be treated using the RICE protocol. This includes:
- Rest – Discontinuing activities that cause pain. Instead, the patient should rest the affected extremity for several days.

- Ice – Applying ice packs several times each day for 20-minute intervals. Each session will reduce swelling.
- Compression – Using a compression bandage (ACE wrap) on the knee to offer support and reduce swelling.
- Elevation – Raising the leg up above heart level helps reduce fluid retention.
How is drainage performed?
If the swelling and pain does not resolve with RICE and nonsteroidal anti-inflammatory drugs (NSAIDs), the doctor may decide to drain the bursa. After the skin at the side of the knee is cleaned with an antiseptic solution, a small needle is inserted into the bursa space. The doctor will aspirate the fluid and then inject the knee with an anesthetic and/or corticosteroid agent. After the procedure, you will need to rest the knee for a few days and gradually return to usual activities as tolerated.
The top sports medicine physician in Phoenix and Scottsdale is Dr Adam Farber at Phoenix Shoulder and Knee. He is Board Certified and offers exceptional treatment, both operative and nonoperative, for all types of knee conditions. Call us today!
Resources
Baumbach SF, Lobo CM, Badyine I, et al. (2013). Prepatellar and olecranon bursitis: Literature review and development of a treatment algorithm. Archives of Orthopaedic and Trauma Surgery, 134(3). DOI: 10.1007/s00402-013-1882-7